Newborn Jaundice: Causes, Symptoms, Treatment, and Prevention
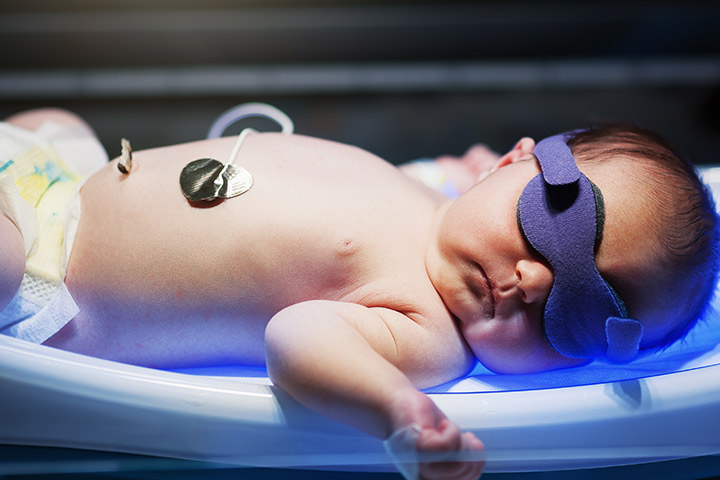
Infant jaundice is surprisingly a common condition that affects about 50% of newborns. The condition is characterised by yellowish coloration of a baby’s skin, and the white part of their eyes.
READ ALSO: See Why Dad of a Newborn 4Qhen, Almost Took His Life
In an otherwise healthy baby born at full-term, infant jaundice is rarely a cause for alarm; it tends to go away on its own. However, if treatment is necessary, infants tend to respond to non-invasive therapy. In rare cases, untreated infant jaundice may lead to brain damage and even death.
The condition is more common among premature babies, and will require more detailed medical attention.
READ ALSO: What You Must Know About Herpes Simplex Infection And Babies
Causes
‘Physiological jaundice’ is caused by a build-up of a chemical called bilirubin in the baby’s blood and tissues. Bilirubin is normally processed by the liver, but a newborn’s liver takes a few days to process it, so about six out of 10 newborns have jaundice to varying degrees.
However, a premature or sick baby or a baby with very high levels of bilirubin will need close monitoring and medical treatments.
Some cases of severe infant jaundice are linked to an underlying disorder; these include:
- liver disease
- sickle cell anemia
- bleeding underneath the scalp (cephalohematoma) – caused by a difficult delivery
- sepsis – a blood infection
- an abnormality of the baby’s red blood cells
- blocked bile duct or bowel
- rhesus or ABO incompatibility – when the mother and baby have different blood types, the mother’s antibodies attack the baby’s red blood cells
- higher numbers of red blood cells – more common in smaller babies and twins
- enzyme deficiency
- bacterial or viral infections
- haemolytic anaemia,
- hepatitis
READ ALSO: Dear MIMsters: How Having Jaundice At Birth Has Affected My Child, Even Three Years After
Symptoms
The most obvious sign of infant jaundice is yellow skin and sclerae (the whites of the eyes). More symptoms of infant jaundice may include:
- drowsiness
- pale stools – breast-fed babies should have greenish-yellow stools, while those of bottle fed babies should be a greenish-mustard color
- poor sucking or feeding
- dark urine – a newborn’s urine should be colorless
Severe jaundice symptoms in infants include:
- yellow abdomen or limbs
- drowsiness
- inability to gain weight
- poor feeding
- irritability
READ ALSO: Beyonce & Jay Z’s Twins Remain Hospitalized After Being Born Premature
Treatment
Typically, treatment for mild jaundice in infants is unnecessary, as it tends to disappear on its own within 2 weeks.
Some treatment options for severe jaundice include:
- Phototherapy (light therapy) – treatment by light rays. The baby is put under a special light, covered by a plastic shield to filter out ultraviolet light. The light manipulates the structure of bilirubin molecules so they can be excreted.
- Exchange blood transfusion – the baby’s blood is repeatedly withdrawn and then replaced (exchanged) with donor blood. This procedure will only be considered if phototherapy does not work because the baby would need to be in an intensive care unit (ICU) for newborns.
- Intravenous immunoglobulin (IVIg) – in cases of rhesus or ABO incompatibility, the infant may have a transfusion of immunoglobulin; this is a protein in the blood that lowers the levels of antibodies from the mother, which are attacking the infant’s red blood cells.
If jaundice is caused by something else, surgery or drug treatment may be required.
Prevention:
The best way to reduce chances of an infant developing jaundice is to make sure they are well fed.
For the first week or so of life, breast-fed babies should be fed 8-12 times a day, while formula-fed babies should be fed 1-2 ounces of formula every 2-3 hours.


